Here is what you’ll find in this week’s newsletter!
Important links 🔗 - the best articles we found this week about the Medicare Market along with links to Jared’s recent LinkedIn posts.
Deep Dive 📚 - 235,000 Duals in Play: MMPs Are Ending in 2026 📊
Sponsor Snapshot 🚀 - brought to you by Modivcare
Compliance Chatter 📢 - Check out the latest regulatory changes.
It’s only a 6 minute read, but it will make you 10x smarter.
Here are IMPORTANT LINKS 🔗 for the week:
Personal Emergency Response Program Reduces Total Cost of Care for Individuals with a History of Falls - (link)
Troy Health, Inc… Admits to Fraudulently Enrolling Medicare Beneficiaries and Identity Theft - (link)
Maryland market threatens to push more Medicare Advantage plans out of the state - (link)
Medicare saved record $2.4B from largest accountable care program last year - (link)
West Virginia system plans ‘substantial’ Medicare Advantage expansion - (link)
As payers stumble, hospitals eye their Medicare Advantage members - (link)
Health insurers face pressure as medical trends accelerate – AM Best - (link)
Medicare Supplement Plan G Continues Its Dominance - (link)
Social Security and Medicare cuts are coming… - (link)
While Others Exit, SCAN Health Plan Enters… - (link)
Jared’s recent LinkedIn posts:
DEEP DIVE 📚
235,000 Duals in Play: MMPs Are Ending in 2026 📊
This AEP already promises to be full of change. Carriers are terminating plans, pulling out of service areas, and shifting benefit strategies (see this year’s Tea Leaves - AEP 2026 🍂 for a rundown).
But there’s another change that hasn’t gotten as much attention: Medicare–Medicaid demonstration plans (MMPs) are going away. These were part of CMS’s long-running experiment to integrate care for dual-eligible beneficiaries. After more than a decade, the demonstration is sunsetting on December 31, 2025 (CMS, CMS-2).
For the ~235,000 beneficiaries still enrolled, and the carriers who serve them, the shift is significant. Let’s break it down.
What Are Medicare/Medicaid Plans?
Back in 2011, CMS launched the Financial Alignment Initiative (FAI) with participating states to test new models for serving people who qualify for both Medicare and Medicaid.
The flagship model was the Medicare–Medicaid Plan (MMP): a three-way contract between CMS, a state Medicaid agency, and a health plan.
Goal: Align Medicare and Medicaid benefits under one umbrella, improve care coordination, and simplify the experience for dual-eligibles.
Design: Capitated payments to a single plan covering primary, acute, behavioral health, and long-term services and supports.
Scale: At peak, 13 states operated MMPs. Today, about 12 states and ~235,000 members remain (MACPAC).
CMS has now decided to transition from temporary demonstrations to permanent integrated D-SNP models (CMS decision memo).
How Members Are Impacted
The demonstration officially ends 12/31/2025. All MMP enrollees will need to move into new coverage for 2026.
States affected: Illinois, Massachusetts, Michigan, Ohio, Rhode Island, South Carolina, Texas, and a handful of others.
Scale: Roughly 235,000 current enrollees.
Carriers: Major players include Molina, Centene, UnitedHealthcare, Humana, Aetna, Commonwealth Care Alliance, Fallon, and regional nonprofits like Neighborhood Health Plan of RI or CareSource (PSM Brokerage).
Here are the impacted states, along with their current MMP enrollment:
State | MMP Enrollment | Total Indiv. MA Enrollment | % of Total |
|---|---|---|---|
Illinois | 75,500 | 773,055 | 10% |
Ohio | 52,432 | 1,163,925 | 5% |
Massachusetts | 39,385 | 477,408 | 8% |
Michigan | 31,364 | 915,594 | 3% |
Texas | 14,064 | 2,116,678 | 1% |
Rhode Island | 11,740 | 137,732 | 9% |
South Carolina | 7,557 | 505,926 | 1% |
New York | 1,687 | 1,768,374 | 0% |
Kentucky | 51 | 382,702 | 0% |
Indiana | 40 | 577,653 | 0% |
Wisconsin | 20 | 591,236 | 0% |
New Hampshire | 11 | 92,276 | 0% |
Total | 233,851 | 9,502,559 | 2% |
—
And here are the impacted Organizations:
Organization | MMP Enrollment | Total Indiv. MA Enrollment* | % of Total |
|---|---|---|---|
Molina | 45,780 | 76,081 | 60% |
CareSource | 41,863 | 66,243 | 63% |
Centene | 33,521 | 487,951 | 7% |
CVS | 32,830 | 960,423 | 3% |
HCSC | 18,267 | 383,819 | 5% |
Humana | 14,078 | 1,531,696 | 1% |
UnitedHealth Grp | 13,930 | 2,782,384 | 1% |
Neighborhood HP of RI | 11,769 | 11,769 | 100% |
Point32Health | 6,861 | 123,327 | 6% |
Independence Health Grp | 5,652 | 5,810 | 97% |
DLP Marquette Gen. | 4,026 | 4,026 | 100% |
Henry Ford Health | 3,587 | 65,167 | 6% |
PHSI | 1,687 | 1,687 | 100% |
Total | 233,851 | 6,500,383 | 4% |
*only including impacted states
What is the plan in each State?
Fortunately, the states aren’t leaving people stranded.
States have been working with carriers to design transition paths into integrated Dual Eligible Special Needs Plans (D-SNPs). Here’s a snapshot of where things stand for some of larger states:
Illinois:
HFS awarded FIDE-SNP contracts to Aetna, Humana, Meridian (Centene), and Molina, with statewide implementation in 2026 and MLTSS (“managed long-term services and support”) fully integrated by 2027 (Becker’s Payer).
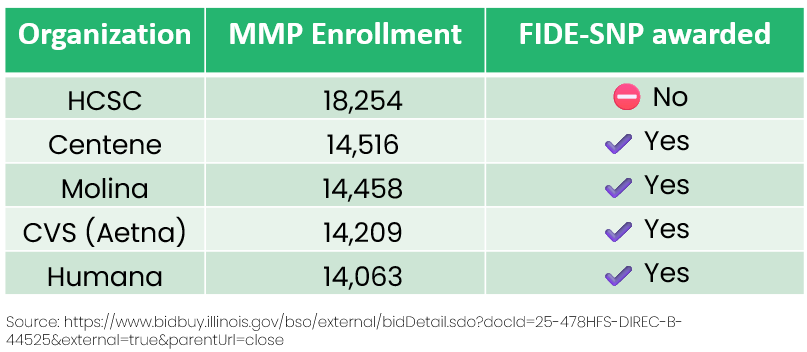
HCSC (who has significant MMP enrollment), and UnitedHealth Group also submitted bids for the new contracts but appear to have not been awarded.
There is some indication that individuals who have MMPs with recently awarded FIDE-SNPs will be crosswalked, and those with HCSC will need to pick a new plan (link).
→ 75,000 duals will be in play, and with HCSC left out of the awards, many members will need new coverage.
Ohio:
Four plans selected — Anthem, Buckeye (Centene), CareSource, Molina — to run the new Next Generation MyCare Ohio starting Jan 1, 2026 (Ohio Medicaid).
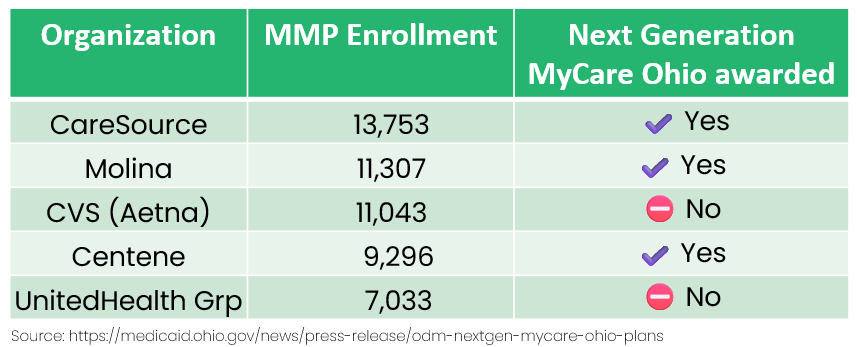
Members with CareSource, Molina and Centene will be crosswalked, while those with CVS and United will need to pick a new plan (or be “auto-assigned”) -(link).
The rollout of this will be phased across counties throughout 2026 (link).
→ Over 52,000 members face change; CVS and United are out, meaning big blocks of auto-assignments or active switches.
Massachusetts:
Massachusetts is moving both One Care (ages 21–64) and Senior Care Options (65+) from demonstration models into FIDE-SNPs effective Jan 1, 2026.
Awarded plans include Commonwealth Care Alliance, Mass General Brigham Health Plan, Point32Health (Tufts), UnitedHealthcare, and Fallon Health (SCO only).
The new contracts (2026–2030) embed exclusively aligned enrollment and maintain One Care’s core features: person-centered care teams, flexible benefits, and integrated appeals.
(Mass.gov, Justice in Aging)
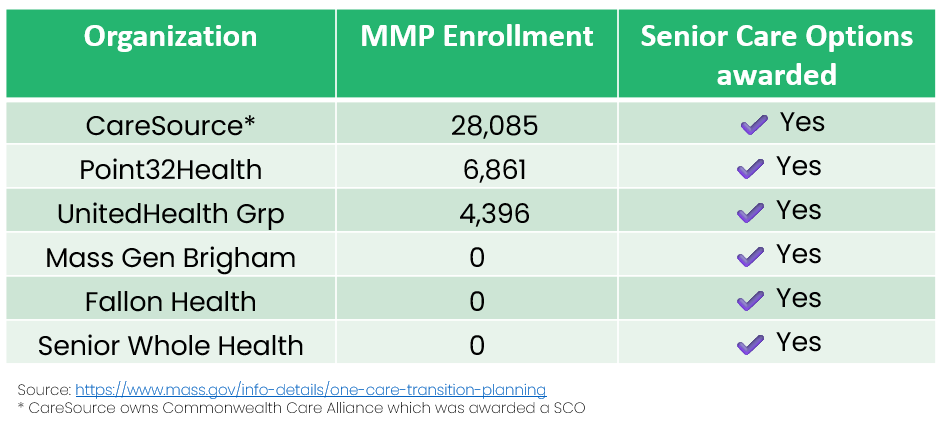
→ Nearly 40,000 duals transition, with multiple plan options
Michigan:
“MI Coordinated Health” launches Jan 1, 2026, with nine plans (Aetna, AmeriHealth, HAP CareSource, Humana, Meridian, Molina, Priority Health, UHC, UPHP). Starts regionally, expands statewide in 2027 (RitterIM, Michigan).
Rhode Island:
All current INTEGRITY MMP members will be crosswalked to the new Neighborhood Health Plan of RI FIDE-SNP on Jan 1, 2026. Members will get new ID cards, continuity of care protections, and an opt-out window (RI EOHHS FAQ).
Texas:
MMP ends 12/31/2025 in demonstration counties.
Integrated D-SNPs tied to STAR+PLUS Medicaid MCOs (e.g., Molina, UHC, Amerigroup/Wellpoint, Superior/Centene, Aetna, Community First) will launch Jan 1, 2026, with expansion statewide in 2027. (Texas, Texas).
Bottom Line
The phase-out of MMPs marks the end of an experiment. But it’s also the start of something more permanent: integrated D-SNPs that are here to stay.
For members, the crosswalk process and continuity rules will help. But many haven’t had to make a plan decision in years. Even if they’re automatically moved, they’ll still need help understanding what’s changing—benefits, networks, and how Medicare and Medicaid fit together.
That’s the opening for agents and carriers. This is a chance to show up for members, explain the changes in plain language, and help them make the move with confidence. Tens of thousands of duals will be in transition, and those who step in to guide them will build trust and long-term relationships.
Disruption in Medicare is nothing new. What matters is how you respond.
SPONSOR SNAPSHOT 🚀: Modivcare
Modivcare is transforming the way members engage in and access their care through remote monitoring and virtual care management. We’re there to help members live more confidently by enabling them to access the care they need to live independently. Our results speak for Modivcare Monitoring’s ability to address cost and close gaps in care across our services.
Learn now Modivcare Monitoring can fit into your members’ coordinated care ecosystem with solutions such as:
Personal Emergency Response Systems (PERS)
Acuity-based vitals monitoring - from digitally-enabled to clinician-led
Medication Management
E3 - Engage, Educate, Empower to address health literacy and support gap closure
Download The Power of PERS White Paper → (Link)
What MMI + Subscribers read this week…
COMPLIANCE CHATTER 📢
Check out this month’s Insurance Regulatory Insights newsletter.
How was today's newsletter?
If you’re ready, here are some ways we can help you:
Did this get forwarded to you? Get the Medicare Market Insights newsletter sent directly to your email weekly:




