This week’s newsletter is Sponsored By: Spark
Learn how to recruit and retain top agents this year → (Get Report)
Here is what you’ll find in this week’s newsletter!
Important links 🔗 - the best articles we found this week about the Medicare Market along with links to Jared’s recent LinkedIn posts.
Deep Dive 📚 - When Plans Go Non-Commissionable: Quantifying the Enrollment Impact
Sponsor Snapshot 🚀 - brought to you by Spark
It’s only a 5 minute read, but it will make you 10x smarter.
Here are IMPORTANT LINKS 🔗 for the week:
2026 Medicare Agent Needs Report - (link)
2026 Medicare Advantage competitive enrollment report - (link)
Ascension CEO ‘taking a closer look’ at Medicare Advantage plans - (link)
Aspirus Health Plan blocked from enrolling Medicare Advantage members as UCare fallout spreads - (link)
Clover Health CEO said company sees opportunity in complex MA environment - (link)
CMS plans sanctions suspending enrollment in Elevance's Medicare Advantage drug plans - (link)
Study suggests AI is boosting hospital billing - (link)
Hospital Indemnity Growth - (link)
Jared’s recent LinkedIn posts:
DEEP DIVE 📚
When Plans Go Non-Commissionable: Quantifying the Enrollment Impact
How do insurance companies slow down sales on Medicare Advantage plans mid-year?
They can’t remove plans from the market, and they can’t change benefits or premiums mid-year.
So the main lever available is commissions.
Historically, carriers have maintained a small list of non-commissionable plans each year. These plans remain available but are not intended to drive new sales.
What’s changed recently is timing. Carriers are now shifting plans from commissionable to non-commissionable mid-year.
UnitedHealth Group (“UHC”) pulled commissions on hundreds of plans mid-2025, and now Humana is doing the same in 2026. Everyone in the industry has an opinion on whether this matters. We went to the data to find out.
How the MA enrollment cycle works:
AEP drives the big enrollment wave (Oct - Dec decisions, showing up in Jan - Feb data).
After that, New to Medicare and SEPs drive smaller monthly changes through the rest of the year.
Agents are the primary distribution channel, and commissions are what drive which plans get presented. This is important because a plan can be technically available but functionally invisible if agents aren't incentivized to sell it.
When commissions are removed, the plan doesn’t disappear, but it often disappears from the sales conversation.
What happens when a plan goes non-commissionable mid-year?
UHC made ~220 plans non-commissionable effective July 1, 2025.
We tracked their enrollment against UHC plans that remained commissionable.
While there are several things that go into enrollment growth (besides commissions), the results are hard to ignore:
Plans that had been growing +2.8% from their post-AEP baseline immediately reversed into sustained monthly declines, losing 18,700 members by December.
Commissionable plans held roughly flat over the same period.
The shift from +2.8% growth to sustained monthly decline represents roughly a 6 percentage point swing, coinciding almost exactly with the commission change.

Note: we observed the same thing for SNP plans. After plans went non-commissionable, the enrollment began a monthly decline.
The AEP Momentum Signal
This is where it gets interesting.
The plans UHC pulled commissions on in July 2025 weren’t underperformers.
They were the hottest plans in the portfolio, with +54% AEP ‘25 growth.
Plans that remained commissionable all year actually shrank during the same AEP.
Type (Non-SNP) | 12/1/2024 | 2/1/2025 | Growth | % Growth |
|---|---|---|---|---|
Commissionable | 4,592,705 | 4,559,149 | (33,556) | -1% |
Non-Commissionable (7/1/2025) | 348,178 | 537,619 | 189,441 | 54% |
Carriers aren't cutting commissions on plans nobody wants. They're cutting them on the plans agents are selling the most, which is what makes the impact so acute.
Enter Humana: April 1, 2026
Humana has announced its own wave of non-commissionable plans, effective April 1, 2026.
The 577K members currently in those plans are sitting on +112% AEP growth. Even more momentum than UHC's plans had last year.
Meanwhile, Humana plans already non-commissionable from January 1 are declining.
Type (Non-SNP) | 12/1/2025 | 2/1/2026 | Growth | % Growth |
|---|---|---|---|---|
Commissionable | 1,684,844 | 2,399,062 | 714,218 | 42% |
Non-Commissionable (1/1/2026) | 2,172,556 | 2,003,669 | (168,887) | -8% |
Non-Commissionable (4/1/2026) | 271,412 | 576,540 | 305,128 | 112% |
So the carrier with the strongest AEP growth in 2026 is now removing commissions from the plans that generated roughly 30% of that growth.
Note: it’s notable that none of the new non-commissionable plans are SNPs.
Bottom Line
Commissions matter more than many industry observers admit. → When commissions were removed mid-year, plans that had been growing immediately shifted into sustained enrollment decline.
Carriers are targeting their fastest-growing plans. → Both UHC (2025) and Humana (2026) removed commissions from plans that drove significant AEP growth.
This is becoming a margin management tool. → Non-commissionable plans allow carriers to slow enrollment growth without changing benefits or exiting markets.
Agents will redirect sales quickly. → When commissions disappear, distribution shifts just as quickly, even when the plan itself remains available.
Expect more of this (for now). → As MA margins tighten, commission changes are likely to become a standard lever carriers use to manage enrollment growth mid-year. I still expect things to eventually settle down, but not quite yet.
Methodology: Analysis at the county-plan level. Enrollment indexed to February 2025 to reflect post-AEP steady-state baseline. July included in the pre-period because enrollment data lags the commission change — July enrollment reflects activity prior to the 7/1 effective date. AEP growth calculated as Dec→Feb enrollment change, capturing the full Annual Enrollment Period effect. "Commissionable during AEP" includes all plans that were commissionable at the time of that AEP, regardless of later commission changes. UHC plans tagged as non-commissionable per carrier commission schedules, matched to CMS monthly enrollment data (Dec 2024–Feb 2026). "Commissionable" = plans not on any non-commissionable or modified commission list for the relevant period. SNP and Non-SNP plans analyzed separately due to differing enrollment dynamics (D-SNPs have continuous enrollment pathways).
SPONSOR SNAPSHOT 🚀: Spark
50% of Medicare agents are ready to leave their upline. It’s not hard to see why.
According to a survey of 500+ agents conducted by Spark and Independent Medicare Network after AEP, here’s what most agencies are still getting wrong:
80% of agents say upline provide quote-and enroll — and little else.
Tech is the #1 factor agents consider when evaluating agencies, but most agencies stop at quote and enroll. Agents want CRMs, automated workflows, and real-time alerts when client coverage changes.
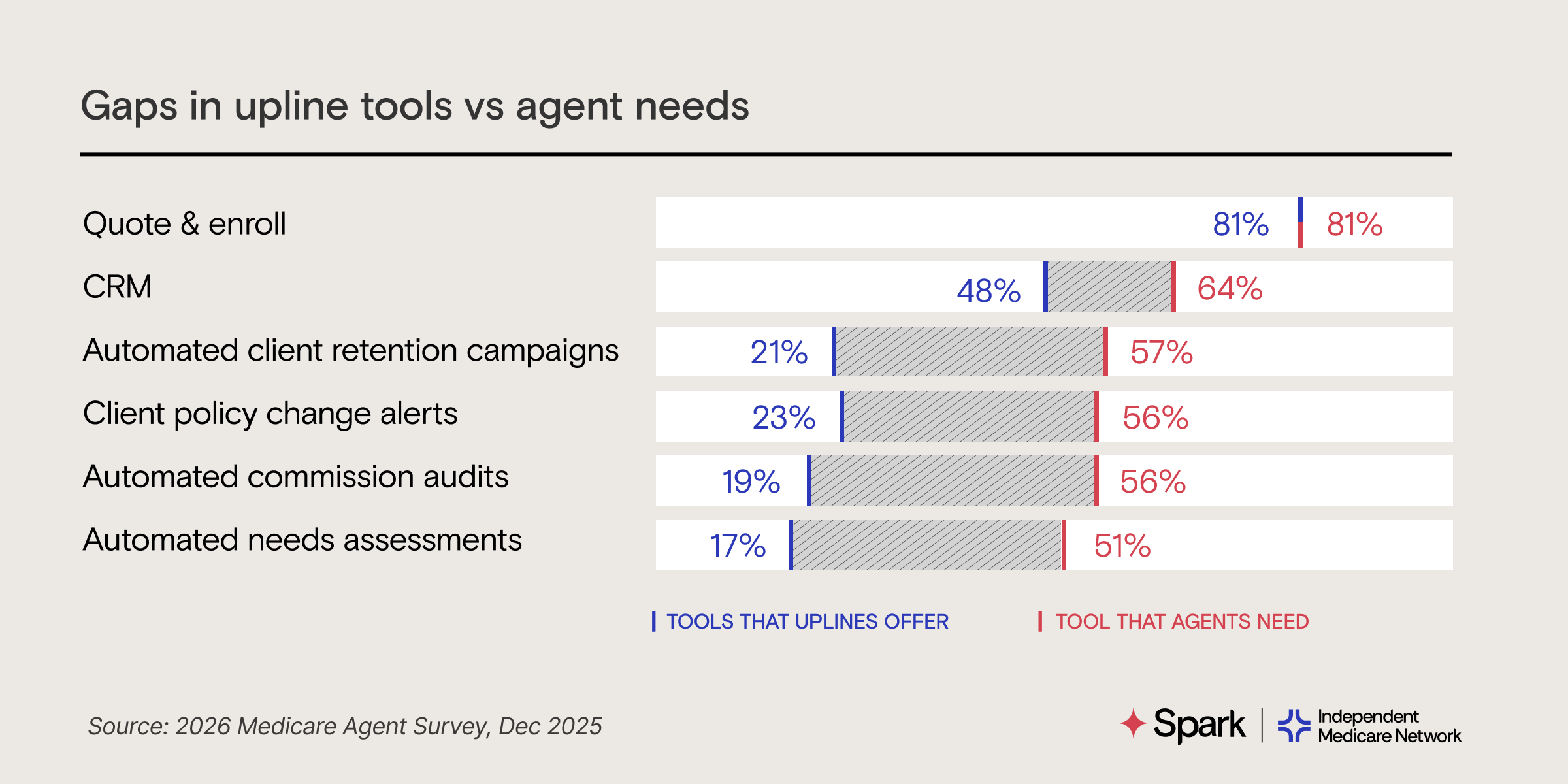
Agents are adapting for the future. Their agencies aren't.
60% say their upline isn't teaching the skills they'll need, like digital marketing and personal branding. Agents are looking for agencies that lead them forward, not ones playing catch-up.

1 in 5 agents are left on their own for marketing, client services, and contracting.
As client books grow, agents get buried in admin work. They want uplines that proactively take back-office work off their hands, so agents can stay focused on building meaningful relationships.
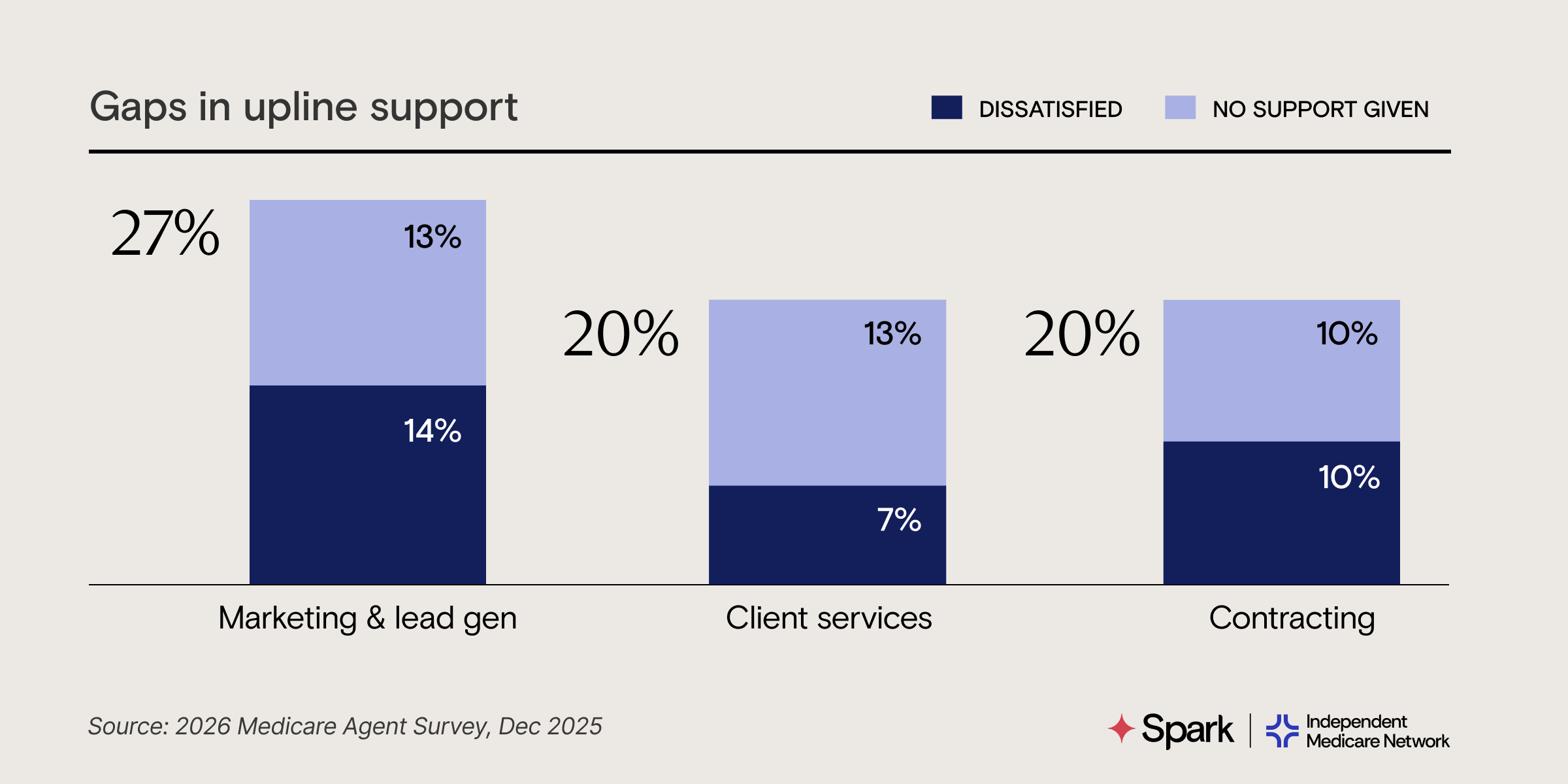
The 2026 Medicare Agent Needs Report breaks down how agencies can win (and keep) top talent in 2026 → Download the full report
What MMI + Subscribers read this week…
Insurance Regulatory Insights March 2026 - New Year, New Bills....a LOT of them (link)
Broker/Agent MA Commissions Expected to Go Up in 2027 - (a preliminary look) - A look at historical MA/MAPD agent comp., and what to expect in 2027. (link)
February ‘26 MA/MAPD and PDP enrollment data - February enrollment data has been loaded. Here are a few observations. (link)
👉 Join TODAY and get 25% off your first 12 months — $75/month instead of $100.
This special AEP Results discount ends March 5.
Receive regulatory updates with the Insurance Regulatory Insights newsletter.
Monthly newsletters providing insight into recent insurance regulatory action
Access to Reg Tracker, a comprehensive list of insurance regulatory actions in all states for this calendar year that are included in the newsletters.
Insurance Regulatory Insights is now included in your MMI+ subscription! You can also subscribe using the link below.
How was today's newsletter?
If you’re ready, here are some ways we can help you:
Did this get forwarded to you? Get the Medicare Market Insights newsletter sent directly to your email weekly:




