This week’s newsletter is Sponsored By: Modivcare Monitoring
Real people caring for your members → Modivcare Monitoring
Here is what you’ll find in this week’s newsletter!
Important links 🔗 - the best articles we found this week about the Medicare Market along with links to Jared’s recent LinkedIn posts.
Deep Dive 📚 - Medicare Advantage Supplemental Benefits: Enrollment Shifts and Carrier Adjustments in 2026
Sponsor Snapshot 🚀 - brought to you by Modivcare Monitoring
It’s only a 5 minute read, but it will make you 10x smarter.
Here are IMPORTANT LINKS 🔗 for the week:
Medicare Base Payment Rates for Hospitals Have Increased While Physician Base Payment Rates Have Declined - (link)
Benefits coverage for no-premium Medicare Advantage plans could drop 50% under 2027 proposed rate: AHIP - (link)
Medicare Advantage’s Discipline Era — and Why the Final Rate Notice Matters More Than It Appears - (link)
AARP, UnitedHealthcare class action alleges wrongful Medicare Supplement claim denials - (link)
Episode 115: Medicare Under Fire featuring Sam Melamed CEO of NCD - (link)
AEP 2026 Medicare Advantage State Deep Dives eBook - (link)
Alleged overpayments to Medicare Advantage plans cost seniors billions: Investigation - (link)
Why are some rural Medicare patients paying more than patients at bigger hospitals? - (link)
Jared’s recent LinkedIn posts:
DEEP DIVE 📚
Medicare Advantage Supplemental Benefits: Enrollment Shifts and Carrier Adjustments in 2026
After a year of significant transition in the Medicare Advantage (MA) market—marked by higher medical loss ratios, more non‑commissionable plans, and widespread plan terminations or service area reductions—it's now possible to see how consumers shifted during AEP.
Previous analyses focused on MA enrollment growth by plan type, geography, and health plan.
This new analysis looks specifically at changes in enrollment in plans with certain supplemental benefits.
First, let’s examine the change in beneficiaries (across both individual MA and SNPs) with access to certain supplemental benefits between February 2025 and February 2026.
Individual MA Plans
Enrollment in plans offering core supplemental benefits—including dental, eye exams, eyewear, hearing exams, hearing aids, and fitness—remained stable, with over 90% of beneficiaries still enrolled in plans providing these services in 2026
Enrollment increased for plans offering acupuncture (+4%) and in‑home support services (+3%).
Several benefits experienced declining enrollment, including fitness (-3%), meals (-6%), remote access technologies (-6%), and telemonitoring (-1%).
The largest declines occurred in over‑the‑counter items (-11%), transportation services (-7%), and devices/home modifications (-11%).

Source: CMS Landscape, Enrollment, and Benefit files for 2025 and 2026 Data excludes employer group health and special needs plans.
—-
Special Needs Plans
Enrollment remained steady for plans offering dental, OTC items, eyewear, eye exams, fitness, hearing exams, hearing aids, telemonitoring, and meal benefits. Notably, fitness and OTC benefits experienced a slight increase in enrollment in 2026.
Enrollment in plans offering in‑home support services grew sharply by 27%, aligning with the expansion of the benefit to more plans (25% of plans in 2026 vs. 17% in 2025).
The most notable decreases were in plans offering transportation services (-8%), devices & home modifications (-7%), and remote access technologies (-7%).

Source: CMS Landscape, Enrollment, and Benefit files for 2025 and 2026
—
Did supplemental benefits impact AEP success? Let’s take a look at supplemental benefits offered by Humana and UnitedHealth Group, the plans with the largest growth and decline in AEP 2026 respectively.
Humana vs. UnitedHealth Group – Individual MA Plans
Humana expanded the number of individual plans offering several supplemental benefits in 2026, reflecting its strong enrollment growth during AEP.
In contrast, UnitedHealth Group (UHC) significantly reduced the number of individual plans offering many of these same benefits, aligning with its enrollment declines.
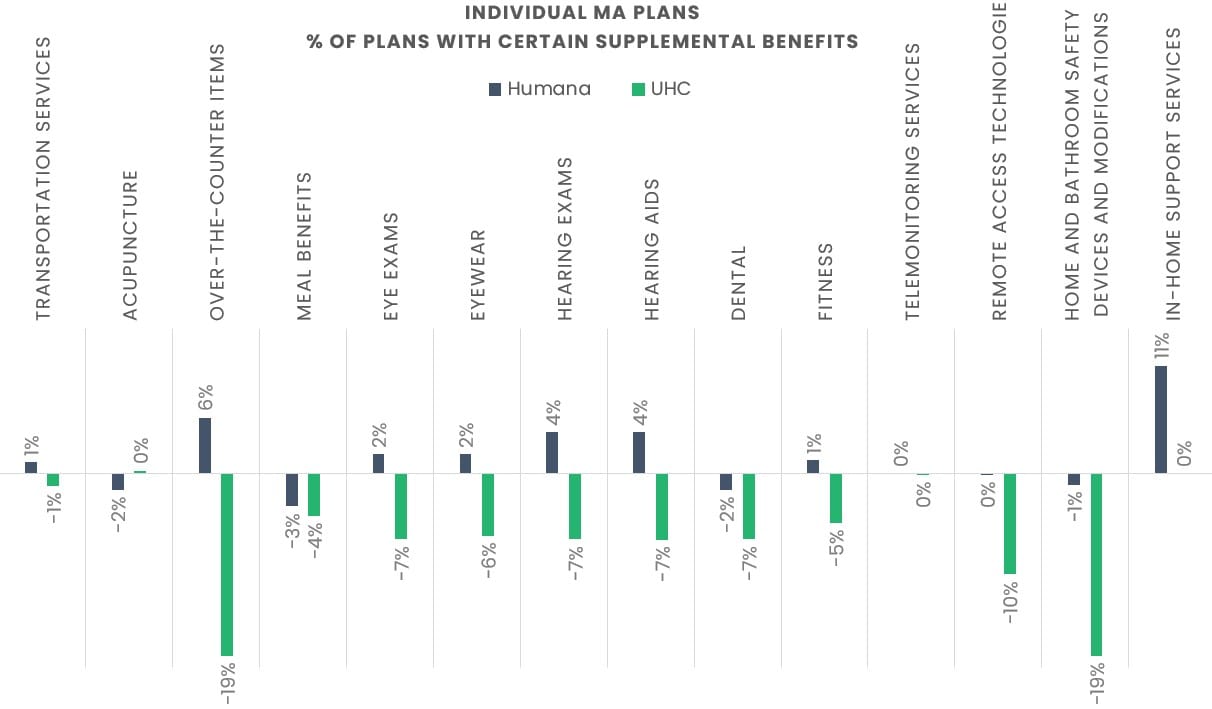
Source: CMS Landscape, Enrollment, and Benefit files for 2025 and 2026 Data excludes employer group health and special needs plans.
—
Humana vs. UnitedHealth Group – Special Needs Plans (SNPs):
The pattern differs for SNPs. Both Humana and UHC reduced the number of SNPs offering several supplemental benefits in 2026.
UHC made the most notable cut, a 10% reduction in SNPs offering remote access technology.
Despite broad reductions in other areas, both companies increased SNP offerings of in‑home support services.
UHC’s jump was especially dramatic, with a 52% increase, indicating a substantial shift in how it structures benefits for its most vulnerable members.
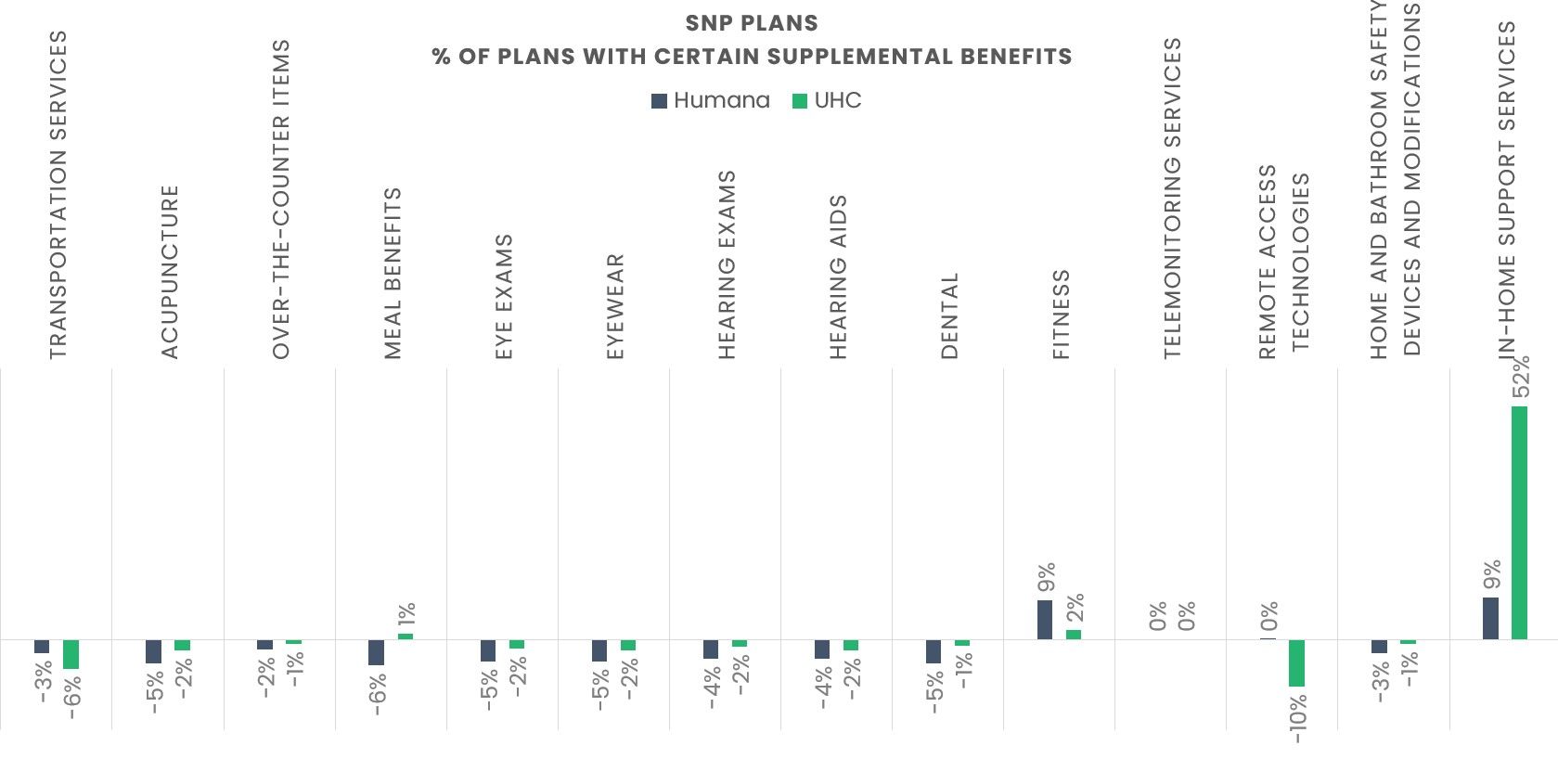
Source: CMS Landscape, Enrollment, and Benefit files for 2025 and 2026
—
As Supplemental Benefit Reporting Requirements and Mid-Year Enrollee Notification of Unused Supplemental Benefits bring more visibility to supplemental benefit utilization and cost to plans, will we see a shift in what supplemental benefits plans are offered in 2027?
SPONSOR SNAPSHOT 🚀: Modivcare Monitoring
Modivcare is transforming the way members engage in and access care through home and community-based solutions. We’re there to help members live more confidently by enabling them to access the care they need - and our solutions deliver: we measurably address cost and close gaps in care across our services.
Learn how Modivcare Monitoring can fit into your members’ coordinated care ecosystem with solutions such as:
Personal Emergency Response Systems (PERS)
Device enabled virtual care management
Medication Management
Community Health Stations
E3 - Engage, Educate, Empower to address health literacy and support gap closure
Saving lives, preserving independence → Modivcare Monitoring
What MMI + Subscribers read this week…
👉 AEP 2026 Medicare Advantage State Deep Dives - Now Available!
How to Get Your Copy:
MMI+ Subscribers → You already have free access!
Download it here → [MMI+ Resources]
Not a “+” Subscriber? You have two options:
1) Purchase for $29
Regularly $49→ [Buy Now]2) [BEST VALUE] Upgrade to MMI+ for $29 for the first month ($100/month after) and get the eBook for free (plus all member benefits) → [Upgrade]
These special AEP Results discounts end March 31.
Receive regulatory updates with the Insurance Regulatory Insights newsletter.
Monthly newsletters providing insight into recent insurance regulatory action
Access to Reg Tracker, a comprehensive list of insurance regulatory actions in all states for this calendar year that are included in the newsletters.
Insurance Regulatory Insights is now included in your MMI+ subscription! You can also subscribe using the link below.
How was today's newsletter?
If you’re ready, here are some ways we can help you:
Did this get forwarded to you? Get the Medicare Market Insights newsletter sent directly to your email weekly:





