This week’s newsletter is Sponsored By: Modivcare Monitoring
Extending access for your most complex populations → (Modivcare Monitoring)
Here is what you’ll find in this week’s newsletter!
Important links 🔗 - the best articles we found this week about the Medicare Market along with links to Jared’s recent LinkedIn posts.
Deep Dive 📚 - AEP 2026: What Plans Are Driving MA Growth Now
Sponsor Snapshot 🚀 - brought to you by Modivcare Monitoring
It’s only a 5 minute read, but it will make you 10x smarter.
Here are IMPORTANT LINKS 🔗 for the week:
2026 Agent Needs Report - See why 50% of all Medicare brokers are looking for a new upline this year.- (link)
Medicare Part D Pharmacy Networks in 2026: Supermarkets Dominate as Drugstores Stall and Independents Walk Away - (link)
2025 Milliman Retiree Health Cost Index - (link)
Weight of the Matter: Obesity’s Financial Impact in Medicare Populations - (link)
Social Security trust fund could run dry earlier than expected, analysis finds - (link)
SCAN launches program to lean on Medicare Advantage brokers as member health navigators - (link)
State of the 2026 Medicare Advantage industry - (link)
Jared’s recent LinkedIn posts:
MA enrollment growth/decline during AEP varied drastically by State. - (link)
February ‘26 MA/MAPD and PDP enrollment data - (link)
MA plans without drug coverage (Part C only) grew enrollment during AEP - (link)
Grateful for great partners - (link)
Cost plan enrollment increases during AEP - (link)
Humana’s turn to “win” AEP - (link)
DEEP DIVE 📚
AEP 2026: What Plans Are Driving MA Growth Now
MA/MAPD enrollment growth slowed during the most recent AEP, continuing a recent trend.
Total MA/MAPD enrollment increased by approximately 110,000 members, compared to 450,000 last year, and over 1 million in prior years.
It’s clear that Health plans prioritized profitability over aggressive enrollment growth.
Why? → Loss Ratios were up and profits were down for Medicare Carriers in 2025 (link).
As a result, fewer consumers switched from original Medicare to MA/MAPD during this AEP than had done so in prior AEPs. In addition, some of the members who had plans terminated likely went back to Original Medicare instead of picking a new MA plan.
Last week we looked at AEP ‘26 enrollment increase by Geography and Health Plan.
This week we are looking at AEP ‘26 enrollment increase by Plan Category & Type.
[As a reminder, the definition of “AEP ‘26 enrollment increase” is the change in enrollment counts from December 2025 to February 2026.]
—
Employer Group vs Individual Plans
All of this year’s AEP growth came from individual plans, while employer group enrollment decreased by ~40,000.
Plan Type | AEP Growth | % Change |
|---|---|---|
Individual (non SNP & SNP) | 149,657 | 0.51% |
Employer Group | -38,519 | -0.67% |
Grand Total | 111,138 | 0.32% |
After a steady increase for a number of years, employer group plan enrollment was flat last year, and saw a slight decrease during this year’s AEP.

source: MA Enrollment Insights web app available to MMI+ subscribers.
—
Plan Type
Similar to last year, this year’s growth was driven by HMO plans which now make up 58% of the market.
This aligns with Carrier’s focus on profitability over enrollment growth as, HMOs typically offer lower costs and better care management compared to PPOs.
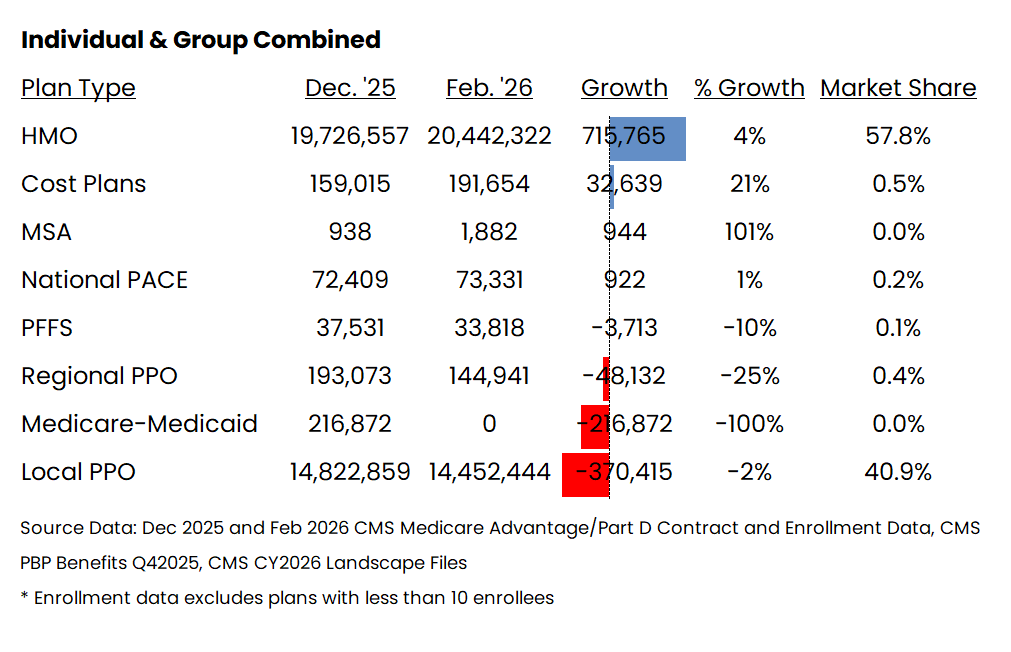
data pulled from MA Enrollment Insights web app available to MMI+ subscribers
As you can see, Medicare-Medicaid plans went away at the end of the year. Most of those members likely ended up in new D-SNP plans in the impacted states.
For example, in the state of IL, ~70,000 members lost their Medicare-Medicaid plans, and D-SNP enrollment grew ~78,000, split between Humana, CVS, Centene, and Molina (the 4 carriers who introduced new FIDE D-SNP products in IL).
—
Plan Category
Special Needs Plans (“SNPs”) once again dominated enrollment growth.
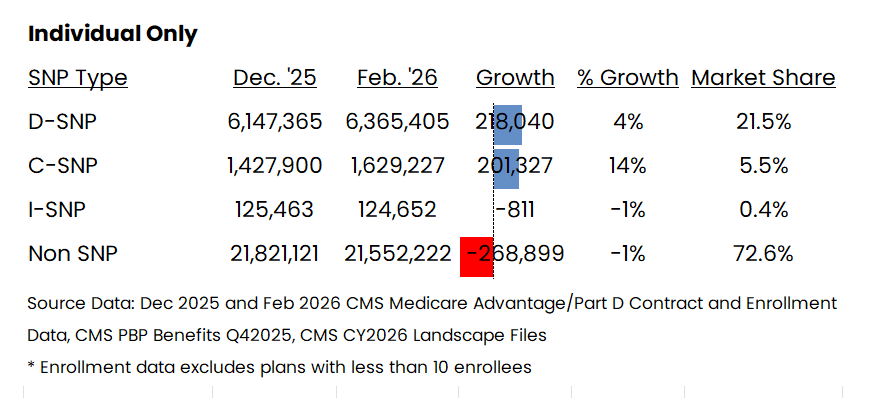
data pulled from MA Enrollment Insights web app available to MMI+
The C-SNP growth continues a trend from last year (~220,000), though the growth this year was spread out among a number of Carriers. Last year’s growth was dominated by UnitedHealth Group.
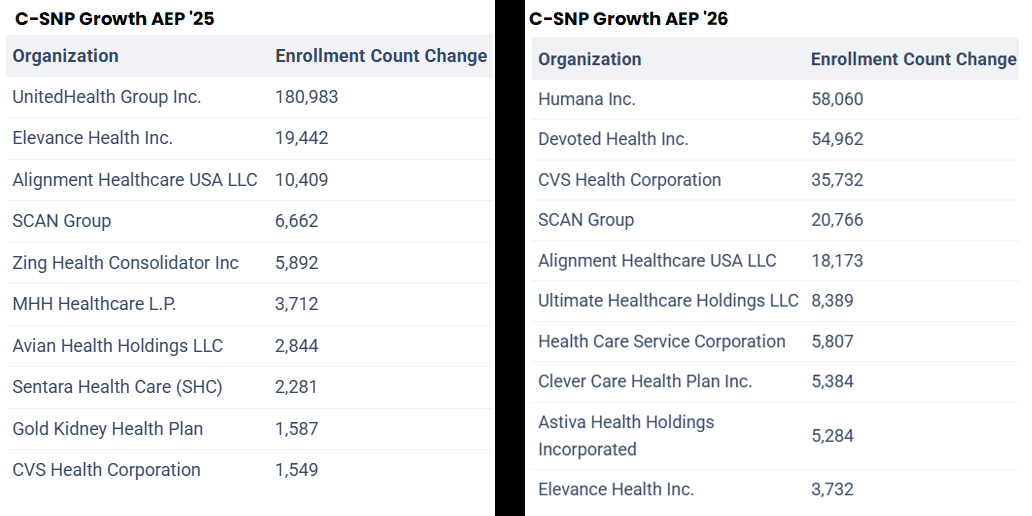
source: MA Enrollment Insights web app available to MMI+ subscribers.
The D-SNP enrollment growth (~218,000) outpaced last year’s growth (~47,000) by a lot. However, most of the D-SNP growth was due to the aforementioned Medicare-Medicaid plan exits.
If you remove the states that were primarily impacted by the MMP plan exits (IL, OH, MI, MA, RI), the D-SNP enrollment growth was a modest ~31,000.
Individual Non-SNP plan enrollment decreased by ~270,000. Some of this is also due to the Medicare-Medicaid plan exits. If you remove those plans from the equation, Individual Non-SNP enrollment decreased by ~52,000.
This is the first time in recent history (or maybe ever?) where Individual Non-SNP enrollment decreased during AEP!
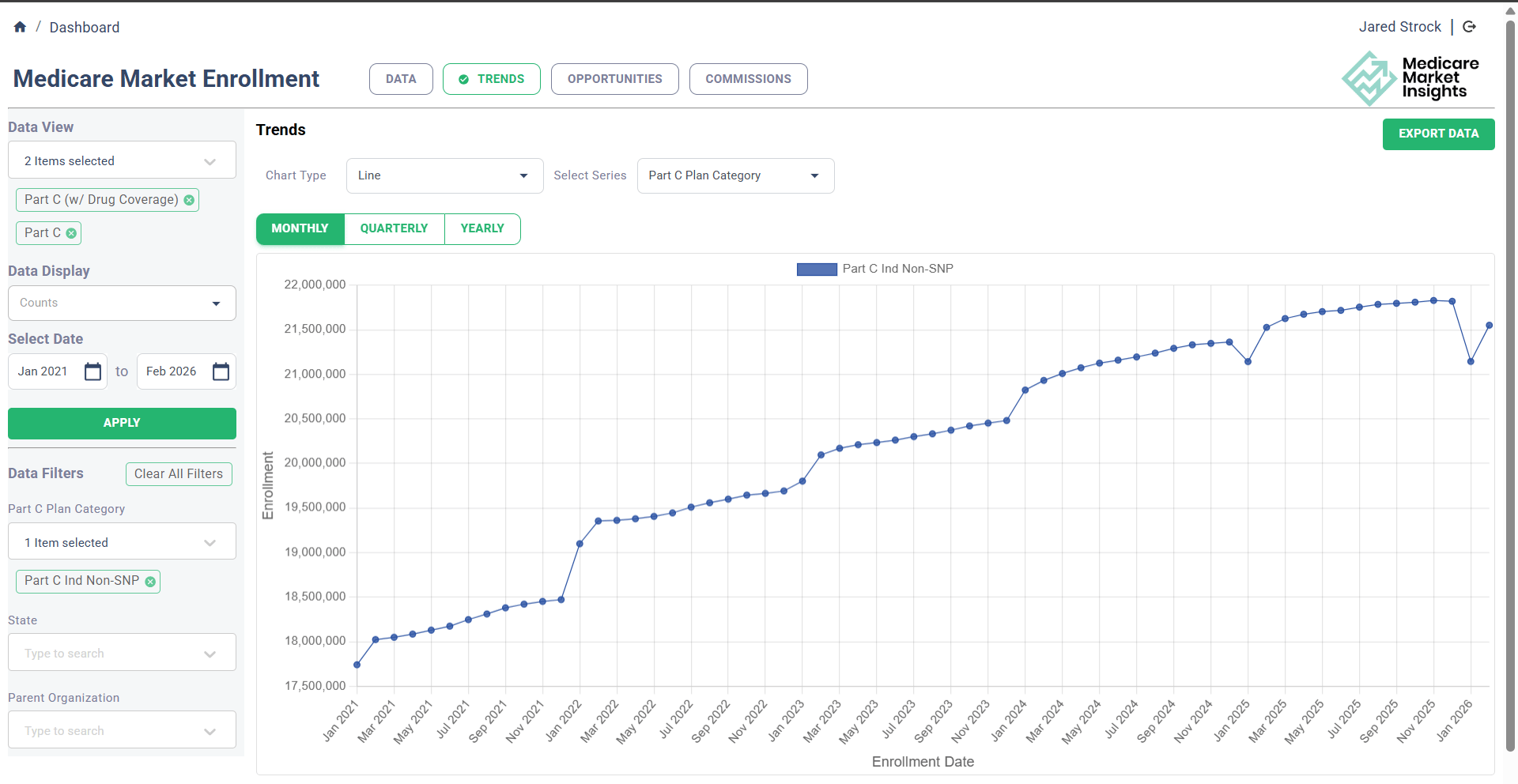
source: MA Enrollment Insights web app available to MMI+ subscribers.
—
Bottom Line
This was a profitability-driven AEP. Carriers prioritized margin protection over aggressive enrollment expansion.
Growth continues to decelerate. MA added ~1M → ~450k → ~110k over the past three AEPs. The slowdown is structural, not random.
SNP growth remains the story, but context matters. A large portion of D-SNP growth was mechanical (MMP transitions), not organic market expansion.
Individual Non-SNP enrollment declined. That hasn’t happened in recent memory. The core retail MA market may be reaching saturation, or at least entering a more competitive equilibrium phase.
HMOs continue gaining share. This aligns with a margin-protection strategy in a higher-utilization environment.
Employer group MA is no longer a growth lever. At least for this AEP.
If 2021–2023 were “growth at all costs,” 2026 marks the shift to “disciplined growth.”
The question for 2027:
Do carriers re-accelerate… or will the trend continue?
SPONSOR SNAPSHOT 🚀: Modivcare Monitoring
Modivcare is transforming the way members engage in and access care through home and community-based solutions. We’re there to help members live more confidently by enabling them to access the care they need - and our solutions deliver: we measurably address cost and close gaps in care across our services.
Learn how Modivcare Monitoring can fit into your members’ coordinated care ecosystem with solutions such as:
Personal Emergency Response Systems (PERS)
Device enabled virtual care management
Medication Management
Community Health Stations
E3 - Engage, Educate, Empower to address health literacy and support gap closure
Saving lives, preserving independence → Modivcare Monitoring
What MMI + Subscribers read this week…
February '26 MA/MAPD and PDP enrollment data - February enrollment data has been loaded. Here are a few observations. - (link)
Insurance Regulatory Insights February 2026 - New Year, New Bills....a LOT of them (link)
Broker/Agent MA Commissions Expected to Go Up in 2027 - (a preliminary look) - A look at historical MA/MAPD agent comp., and what to expect in 2027. (link)
👉 Join before March 5th and get 25% off your first 12 months — $75/month instead of $100.
This special AEP Results discount ends March 5.
Receive regulatory updates with the Insurance Regulatory Insights newsletter.
Monthly newsletters providing insight into recent insurance regulatory action
Access to Reg Tracker, a comprehensive list of insurance regulatory actions in all states for this calendar year that are included in the newsletters.
Insurance Regulatory Insights is now included in your MMI+ subscription! You can also subscribe using the link below.
How was today's newsletter?
If you’re ready, here are some ways we can help you:
Did this get forwarded to you? Get the Medicare Market Insights newsletter sent directly to your email weekly:




