This week’s newsletter is Sponsored By: EnrollHere
Run insurance distribution with confidence → EnrollHere
Here is what you’ll find in this week’s newsletter!
Important links 🔗 - the best articles we found this week about the Medicare Market along with links to Jared’s recent LinkedIn posts.
Deep Dive 📚 - What's in a Medicare Advantage Medical Loss Ratio?
Sponsor Snapshot 🚀 - brought to you by EnrollHere
It’s only a 5 minute read, but it will make you 10x smarter.
Here are IMPORTANT LINKS 🔗 for the week:
Humana's NTM Commission Change - (link)
Aetna Agrees to Pay $117.7 Million to Resolve False Claims Act Allegations - (link)
CMS Announces Manufacturer Participation in Third Cycle of Medicare Drug Price Negotiation - (link)
The Quiet Power Shift Inside Medicare Supplement - (link)
Pennsylvania holds special Medicare enrollment period due to LVHN and United dispute - (link)
Medicare Advantage 'dark money' group tries to win higher payments for insurers - (link)
Most Medicare Beneficiaries Affected by Plan Terminations in 2025 Have Robust Medicare Advantage Options in 2026 - (link)
Medicare Supplement - Trend Components - (link)
Jared’s recent LinkedIn posts:
DEEP DIVE 📚
What's in a Medicare Advantage Medical Loss Ratio?
If you've been paying attention to the Medicare Advantage market recently, you've heard the same word over and over: MLR.
Medical Loss Ratios (“MLR”) in Medicare Advantage have been elevated for two consecutive years (UHC historical MLRs, Carrier side-by-side).
Carriers have responded. Plan terminations, benefits cut heading into AEP, plans shifted to non-commissionable status mid-year to slow enrollment. The financial pressure is reshaping the market.
What's missing from most conversations is a clear picture of what actually makes up an MA MLR - which is more complex than most people realize - and whether plans that grow rapidly during AEP end up with higher MLRs.
We went to the CMS public data to find out.
A note on the data and process: CMS publishes contract-level MLR data annually. The most recent year available is CY 2023, and it's the most granular public release CMS has ever produced as 2023 was the first year CMS required detailed supplemental benefit reporting, giving us visibility into the MLR anatomy that simply didn't exist in prior years. CY 2024 and 2025 data will be released in coming years, and we'll update this analysis when they are. Given what happened in the MA market in those years, that data will be worth watching closely.
Data analysis for this piece was built with the assistance of Claude (Anthropic). Methodology, data and conclusions are my own.
The Revenue Side
The denominator of the MLR is Revenue. Here is what revenue looked like for MA contracts in 2023.

84 cents of every dollar flowing into an MA contract comes from CMS capitation.
Everything else, member premiums, Part D subsidies, rebates, is relatively small.
MA economics are fundamentally a government payment model, not a premium pricing model. A plan's financial performance lives or dies on how well its bids match actual member costs in each market.
Note: The Inflation Reduction Act’s impacts to Part D will likely shift what this looks like in 2025 forward.
The Claims Side
The numerator of the MLR is claims. Here is what claims looked like for MA contracts in 2023.

Across 635 MA contracts, total claims in 2023 were $485.3 billion.
A&B medical claims are 72.6% of the total (inpatient, outpatient, physician services, etc.).
Part D Rx adds another 20.6%.
Another 5.1% is Supplemental Benefits.
This is the first year CMS published a detailed sub-category breakdown, and the numbers tell a story.
Dental leads at $6.6B (27% of supplemental spend), but the second-largest bucket is "Non-Primarily Health Related — Other" at $5.2B. OTC items add $4.5B.
While supplemental benefits only make up 5.1% of spend, they are often the main benefits marketed to seniors, and likely a big driver of plan switching.
The 2023 MLR Landscape

The aggregate market MLR was 90.7% in 2023. The median contract sat at 91.0%. The regulatory floor is 85%. Only 17 contracts (3%) fell below it.
110 contracts (17% of the market) reported MLRs above 100%. One in six MA contracts lost money on their medical business in 2023.
Another third of the market sat in the 90–95% zone, leaving almost no margin for utilization surprises. A plan can have a 90% MLR and still lose money once admin costs are layered in, and admin costs average 8% of revenue across the market.

A few segment observations worth noting. Local PPOs had higher MLRs than HMOs (92% median vs. 91%). Non-SNP individual contracts were the most stressed segment at a 93% median MLR.
Do the Contracts That Grow the Most End Up With Higher Loss Ratios?
Plans that grew the most during AEP 2023 were almost by definition the ones with the most aggressive benefit designs: high OTC allowances, flex cards, low or $0 premiums. Those same benefit designs tend to attract higher-cost members and leave less margin to absorb utilization.
The question isn't whether growth caused the high MLR. It's whether the contracts that grew the most also ended up with the worst loss ratios.
In 2023, they did.
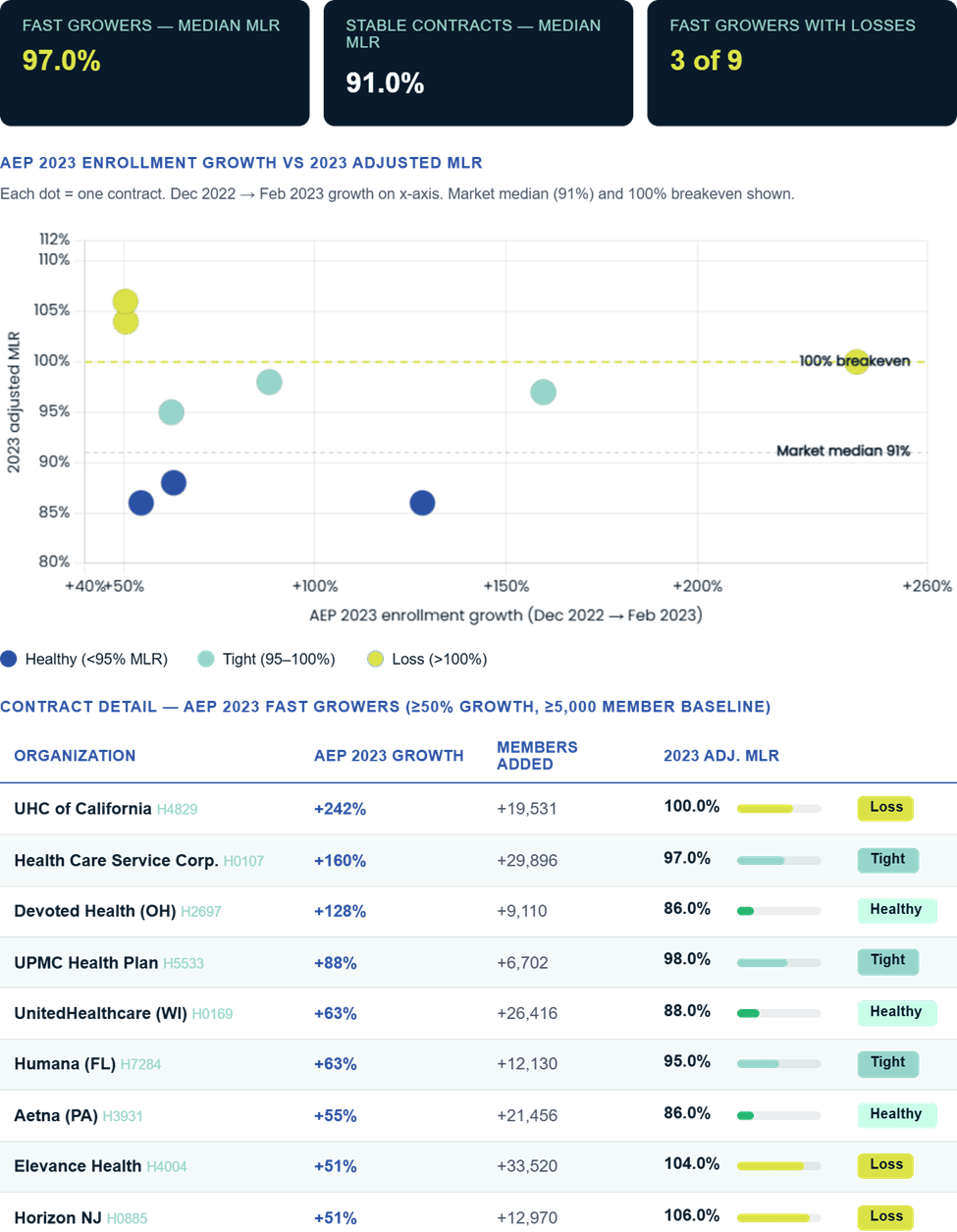
Fast-growing contracts (≥50% enrollment growth, ≥5,000 member baseline) posted a median adjusted MLR of 97.0%, vs. 91.0% for stable contracts. Three of nine fast growers reported MLRs above 100%, versus 8% of stable contracts.
Growth and high MLR are both outputs of the same upstream decision, the product design that won members was the same product design that generated elevated claims.
CY 2024 and 2025 data will be fascinating to analyze as 2023 was a fairly normal year.
Bottom Line
MA MLR is more complex than it looks. → 84% of revenue is government capitation. The claims side includes supplemental benefits, provider incentive pools, and quality improvement expenses, none of which appear in a traditional insurance MLR. The 2023 CMS data is the most granular public release ever, and it sets an important baseline as carriers roll back benefits in 2024 and 2025.
Compliance with the 85% floor and profitability are not the same thing. → 17% of contracts ran above 100% MLR in 2023. Another third sat in the 90–95% range with almost no margin cushion. When you layer in 8% average admin costs, a lot of those contracts were losing money.
The contracts that grew the most in AEP 2023 also had the worst loss ratios. → The 6-point median MLR gap between fast growers and stable contracts is real. The likely explanation is product design, the same benefit aggressiveness that drove enrollment also drove claims.
The next two data releases will be fascinating. → CY 2023 reflects a fairly normal MA market. The CY 2024 and CY 2025 MLR data will be fascinating to analyze.
SPONSOR SNAPSHOT 🚀: EnrollHere
EnrollHere is the system of record for modern insurance distribution, giving carriers and agencies unified operational control across sales, commissions, compliance, and performance.
We replace fragmented technology stacks with a single, closed-loop operating platform that delivers end-to-end visibility across the distribution lifecycle, commission accuracy aligned to carrier truth, and accountable distribution oversight.
Learn how EnrollHere can strengthen and simplify your distribution ecosystem with solutions such as:
• Unified sales and lead flow management
• Commission tracking aligned to carrier payment truth
• Policy-level visibility across the lifecycle
• Hierarchy and partner management at scale
• Audit-ready compliance and performance intelligence
Distribution under operational control → Explore EnrollHere
What MMI + Subscribers read this week…
March ‘26 MA/MAPD and PDP enrollment data - February enrollment data has been loaded. Here are a few observations. (link)
Humana's NTM Commission Change - Estimating the impact of prorated New-to-Medicare commissions on carrier expense and distributor LTV. (link)
Insurance Regulatory Insights March 2026 - New Year, New Bills....a LOT of them (link)
New in MMI+ : New Plan Type Visual and Filter by Contract & Plan ID (link)
👉 AEP 2026 Medicare Advantage State Deep Dives - Now Available!
How to Get Your Copy:
MMI+ Subscribers → You already have free access!
Download it here → [MMI+ Resources]
Not a “+” Subscriber? You have two options:
1) Purchase for $29
Regularly $49→ [Buy Now]2) [BEST VALUE] Upgrade to MMI+ for $29 for the first month ($100/month after) and get the eBook for free (plus all member benefits) → [Upgrade]
These special AEP Results discounts end March 31.
Receive regulatory updates with the Insurance Regulatory Insights newsletter.
Monthly newsletters providing insight into recent insurance regulatory action
Access to Reg Tracker, a comprehensive list of insurance regulatory actions in all states for this calendar year that are included in the newsletters.
Insurance Regulatory Insights is now included in your MMI+ subscription! You can also subscribe using the link below.
How was today's newsletter?
If you’re ready, here are some ways we can help you:
Did this get forwarded to you? Get the Medicare Market Insights newsletter sent directly to your email weekly:




